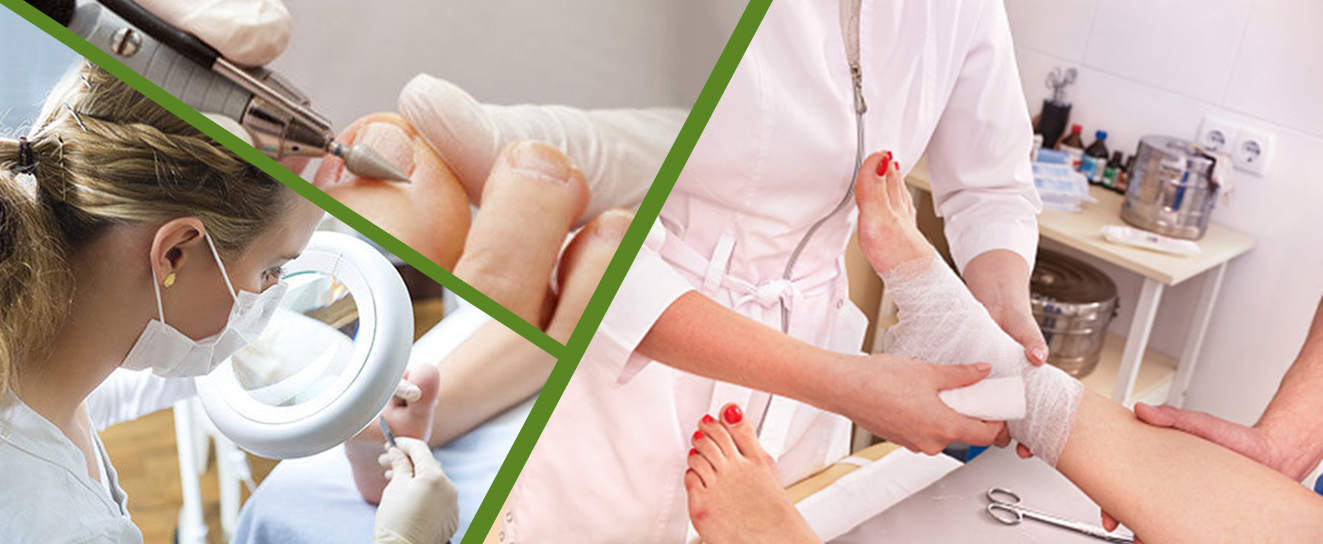
Healthy feet and legs enhance mobilty and quality of life. Most of us have been given the gift of mobility and our aim is to promote this and keep you active and pain free throughout your life.We pride ourselves on patient education. We want you fully informed to make the best from your treatment options.

Primary Foot Care
Primary foot care addresses common nail and skin complaints of the foot. This is a physical form of treatment involving cutting and filing nails and the reduction of thickened skin followed in most cases by the application of skin emollients to keep the skin soft and supple. Antibiotics and topical and/or oral anti-fungal medications can be prescribed to treat skin and nail infections.
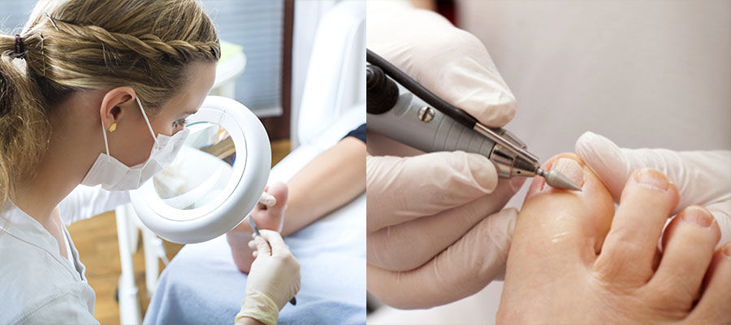
Primary foot care can be used to address:
Primary foot care can dramatically improve the comfort and appearance of your feet.
- Corns and callous (including cracked heels)
- Chronic or acute ingrowing toe nails
- Ulcer debridement/wound care (common in diabetic patients)
- Drainage of skin abscesses and sinuses (common in diabetic patients)
- Management of skin and nail mycotic infections (fungal infections)(common to patients over 60 years of age)
Ortho-Mechanical Treatment (including foot orthoses/orthotics)
- Foot orthoses (prefabricated, custom made or a hybrid of these two designs)
- Footwear (Off the shelf designs or custom made)
- Paddings (supportive and deflective – an excellent temporary intervention – custom made and prefabricated designs are available)
- Strappings (provide support and compression – are both diagnostic and offer excellent temporary pain relief)
- Foot and ankle immobilisation boots (walking boots)
- Toe padding and supports (both custom made and prefabricated designs are available)
Physical Therapy
The specialists at ACT Podiatry can provide advice on and/or administration of stretching exercises, strengthening exercises and massage therapy.
Physical therapy includes the RICE principal:
- Rest
- Ice
- Compression
- Elevation
(NB: Referral to a physiotherapist may be required for complex cases).
Pharmacology
There are 7 classes of drugs available to podiatric practitioners who have achieved endorsement status as recognised by the Australian Health Practitioner Regulatory Authority and the Australian Podiatry Association. Medications are very important to address pain and infection and can be used as an adjunctive with other forms of treatments.
Medications used by endorsed podiatric practitioners are:
- Anti-inflammatory medication (NSAIDS, corticosteroids)
- Analgesics [pain killers – including codeine phosphate, paracetamol, Endone (podiatric surgeons only), NSAIDS, corticosteroids]
- Oral antibiotics (treatment for bacterial infections)
- Oral anti-fungals (oral Lamisil can be prescribed with monitoring from your GP)
- Anxiolytics and sedatives (used for the treatment of anxiety associated with treatment)
- Local anaesthetics (used to eliminate pain associated with a procedure, can also be used diagnostically and therapeutically)
- Anti-emetics (anti-nausea – used to eliminate the feeling of nausea commonly associated with some medications such as codeine or related to anxiety)
(NB: Referral to a medical practitioner may be required in certain cases)
Minor Clinical Procedures
Nail Surgery
Nail surgery is effective at permanently eliminating pain or infection associated with acute or chronically ingrowing +/- thickened toe nails. Surgery eliminates the need for repeated consultations to remove the offending nail spicule/s and the constant use of antibiotics to manage infection.
The pain associated with nail surgery is usually minimal, but if this a concern medications can be purchased over the counter or prescribed. Sometimes antibiotics need to be used in the management of ingrowing toe nails, either before or after surgery.
Verrucae/Plantar Wart Curettage
Verrucae curettage (or surgical excision of plantar warts) is a highly reliable and effective technique at eliminating the pain associated with plantar warts or eliminating their growth and spread. Post- operative pain associated with this can be considerable, as plantar warts are almost always present on the weight bearing areas of the foot. However, much comfort can be achieved with an appropriate post-operative dressing, shoes and the use of oral analgesia (pain killers). It is advisable to reduce the level of weight bearing activity for a week or so following this procedure.
Plantar warts are very common and can be treated permanently with a surgical excision.
Wound Care
This is a critical form of treatment for those patients with chronic wounds, most commonly found in the diabetic population but also patients with peripheral neuropathy, peripheral arterial or venous disease and patients who are immunosuppressed (i.e. rheumatoid arthritics). Our management will commence with a thorough medical history, identification of the underlying cause and assessment of your wound. The objective of wound care management is to eliminate the risk of infection, treat it if it is present and ultimately heal the wound. Wound care may involve a variety of health care providers.
Techniques include:
- Wound drainage and debridement
- Paddings and dressings
- Foot orthoses and other ortho-mechanical devices (i.e. digital padding, foot and ankle braces, walking boots)
- Management of infection (oral or intravenous antibiotics with general medical practitioner or other specialist involvement as required and often soft tissue debridement which reduces the level of bacterial wound contamination).
- Referral as required to vascular or other specialists
Referral
In some instances referral is an appropriate form of management. A multidisciplinary approach is often important particularly when managing complex cases. It is common for patients with complex complaints and with diabetes and arthritis to seek advice and treatment from multiple practitioners.
We commonly refer to:
- General medical practitioners
- Medical imaging specialists
- Physiotherapists
- Massage therapists
- Chiropractors
We also refer to:
- Vascular surgeons
- Orthopaedic surgeons
- Sports physicians
- Pain medicine specialists
- Other medical specialists (i.e. dermatologists)
foot and ankle conditions
- Hallux Valgus (Bunions – progressive dislocation of the big toe joint)
- Hallux Rigidus (Osteoarthritis of the big toe joint)
- Hammer/Claw Toes
- Plantar Forefoot Pain
- Heel Pain (including plantar fasciitis/plantar fasciopathy)
- Bumps and Lumps (bony and soft tissue)
- Arthritis (forefoot, midfoot, rearfoot and ankle)
- Complex foot and ankle complaints (patients with multiple concerns)
- Ingrown Toenail Surgery
- Something Unusual
faq
- What are Podiatrists & Podiatric Surgeons?
- What is the point of difference between
ACT Podiatry and other practices? - What are common forefoot conditions
treated at ACT Podiatry? - What are common mid-foot and rear foot
conditions seen at ACT Podiatry? - What predisposes a person
to lower limb pain - What are foot orthoses?
- Can a spinal condition cause foot pain?
- Is arterial disease a cause of foot pain?
- I am diabetic and my feet burn
– what is this? - Can in-growing toe nails and plantar warts be cured?
Suite 8 (Ground Floor), 146 Scollay St, Greenway ACT 2900
6287 4889
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Suites 16-17 (First floor) 14-16 Brierly St, Weston ACT 2611
6287 2818
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Copyright © 2018, ACT PODIATRY | SEO by High Jump Digital

